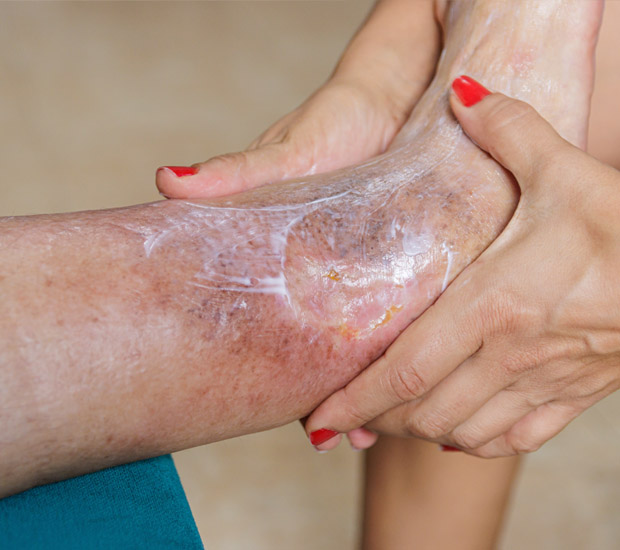
Vascular UlcersDowney, CA
Vascular ulcers are chronic wounds that develop due to poor blood circulation. They typically affect the legs, ankles, and feet. These ulcers can be painful, slow to heal, and prone to infection, which can impact an individual’s overall health. Fortunately, we offer minimally invasive treatment options that can address circulatory issues at their source, preventing severe complications and restoring the patient’s quality of life.
At ProVascularMD, we address the root cause of vascular ulcers from the inside out. We use advanced imaging to navigate your vascular system and restore the blood flow that your body needs to heal. Do you have questions for our team? Reach out to our Downey office today by calling (310) 341-4867 to schedule a consultation.
Understanding Vascular Ulcers
Vascular ulcers are chronic wounds that develop when a person’s blood circulation is compromised, limiting the delivery of oxygen and nutrients that tissues need to repair themselves. This impaired circulation can result from damage or dysfunction of the blood vessels, leading to breakdown of the skin and underlying tissues over time. Unlike temporary (acute) wounds, vascular ulcers often persist for weeks or months and become increasingly difficult to heal without professional medical treatment.
Vascular ulcers are common, particularly as people get older. According to the Cleveland Clinic, about 1% of adults have a vascular ulcer. For older adults above the age of 65, the numbers increase to 3-5%.
“Unlike temporary (acute) wounds, vascular ulcers often persist for weeks or months and become increasingly difficult to heal without professional medical treatment.”
Arterial vs Venous Ulcers
In the human body, arteries and veins consistently work together to bring blood towards and away from different areas. However, dysfunction in either part of the vascular system can lead to vascular ulcers. There are two primary types of vascular ulcers: arterial and venous.
Arterial ulcers
Arterial ulcers, also known as ischemic ulcers, are caused by peripheral arterial disease (PAD), where the arteries delivering oxygen-rich blood to the lower extremities become clogged with plaque accumulation. The hardening of the arteries limits the forward flow of the blood. When the skin and muscles are deprived of oxygen and nutrients, the tissue begins to die, and even a tiny scrape can turn into a deep, non-healing wound.
Medical professionals often find ulcers on pressure points of the foot, such as the tips of the toes, between the toes, or on the ankles. These areas are common since they are the furthest from the heart. If a person with PAD develops an injury on their foot, there is an increased risk of the wound evolving into an arterial ulcer.
Venous Ulcers
Venous (stasis) ulcers are the most common type of venous wounds. They occur when the veins in the legs fail to deliver blood toward the heart. Instead, the blood begins to pool in the lower leg and create pressure in the veins, leading to fluid leakage, skin inflammation, and eventually, a breakdown of the skin tissue.
Venous ulcers often appear irregularly shaped, with the skin around the wound being hard or discolored. Patients may experience a dull ache, inflammation, or itching in their legs. The wound may also emit a foul odor or pus.
“There are two primary types of vascular ulcers: arterial and venous.”
Risk Factors for Vascular Ulcers
While some individuals have an increased risk of venous or arterial disease due to their genetics, most ulcers develop when multiple risk factors combine to restrict blood flow or weaken vessel walls. When diagnosing vascular ulcers, a vascular and interventional radiologist (VIR) will identify the underlying cause of the wound by evaluating the patient’s vascular and overall health.
Depending on whether the ulcer is arterial or venous, risk factors of vascular ulcers include:
- Diabetes
- High cholestrol levels
- High blood pressure
- Aging
- Smoking and other tobacco use
- Being overweight or obese
- A history of blood clots
- Chronic venous insufficiency (CVI)
- Peripheral vascular diseases
Many of these risk factors can progress without visible symptoms and can go undetected until it is too late. In some cases, an untreated vascular ulcer can lead to serious complications, including the patient losing their limb. The sooner that the VIR can diagnose and treat the cause of the vascular ulcer, the better the treatment outcome.
“While some individuals are genetically predisposed to venous or arterial disease, most ulcers develop when multiple risk factors combine to restrict blood flow or weaken vessel walls.”
Vascular Ulcer Treatment Options
The goal of vascular ulcer treatment is to re-route blood flow through healthy arteries and veins nearby. The chosen treatment depends on the severity of the wound. The VIR may recommend making lifestyle changes and taking medications for patients with smaller ulcers. Additionally, they may have the patient wear compression stockings to help improve venous blood flow.
However, if a more conservative approach does not work and the ulcer does not heal or gets bigger, the VIR may recommend a minimally invasive procedure known as revascularization to restore blood flow the the affected area. During this procedure, the VIR uses real-time imaging to navigate a catheter through a pinhole incision. They may use different tools to open the vascular system, such as angioplasty, thrombectomy, and stenting. This minimally invasive method restores internal blood flow and encourages the ulcer to heal.
“The goal of vascular ulcer treatment is to re-route blood flow through healthy arteries and veins nearby.”
Preventing Vascular Ulcers
To prevent vascular ulcers, patients need to start by preventing vascular issues. While some of these issues are unavoidable due to genetics, many are preventable by practicing habits that promote healthy blood flow in the legs and feet. Simple lifestyle changes can improve blood circulation, reducing the risk of vascular ulcers. These habits include:
- Avoiding smoking and tobacco use
- Maintaining a healthy weight
- Engaging in regular, low-impact exercise
- Elevating legs after standing all day
- Wearing compression stockings to reduce swelling and blood pooling
Proactive habits help improve the patient’s vascular system and overall health, supporting resilient skin and blood flow. When combined with professional treatment from a VIR, these daily actions serve as a defense against future or recurrent vascular issues.
“Simple lifestyle changes can improve blood circulation, reducing the risk of vascular ulcers.”
Questions Answered on This Page
Q. How common are vascular ulcers?
Q. What is the difference between venous and arterial ulcers?
Q. Who is more likely to develop vascular ulcers?
Frequently Asked Questions about Vasscular Ulcers
Q. How can I tell if my leg sore is a vascular ulcer?
A. If you have a wound on your lower leg, ankle, or foot that has not improved in two to four weeks, it is likely a vascular issue. You may also notice surrounding skin is discolored, swollen, or leathery, along with a persistent aching or heaviness in the limb. Fortunately, a quick, noninvasive imaging test at our Downey office can confirm whether your vascular system is the primary cause of the wound.
Q. Can vascular ulcers come back after treatment?
A. While our procedures are highly effective at fixing the root cause of vascular ulcers, vascular disease is a chronic condition that requires long-term management. By addressing the symptoms early, Dr. Michael Lalezarian, MD, reduces the chance of the ulcer recurring in the same spot. The ProVascularMD team will provide you with a treatment plan tailored to your needs, which may include compression therapy or lifestyle changes, to keep your legs and feet healthy for the foreseeable future.
Q. Will I have large scars or need switches?
A. One of the benefits of interventional radiology is that we work through a tiny nick in the skin, typically no larger than a grain of rice. Our instruments are small, so most patients will not need traditional stitches. There is virtually no scarring afterward. After treatment, you can leave the office with nothing more than a small adhesive bandage over the surgical site.
Q. How long will it take for the ulcer to close?
A. While we can restore your blood flow within a couple of hours, the skin itself needs additional time to regenerate. Most people will notice changes in the color and drainage of their wound within the first 7 to 10 days after the procedure.
Q. What are the risks of vascular ulcer treatment?
A. While no medical procedure is entirely without risk, vascular ulcer treatment by a VIR has a lower complication rate than open surgery, as we do not use large incisions or general anesthesia. That said, minor risks include bruising at the entry site or a reaction to the contrast dye. The ProVascularMD team takes every precaution to protect your comfort and safety. If you have questions or concerns about your procedure, do not hesitate to contact us.
Find Relief Today
At ProVascularMD, we provide minimally invasive treatment to heal vascular ulcers. Our VIRs offer a range of minimally invasive techniques in the Downey area to treat arterial and venous vascular ulcers. Are you ready to find relief from vascular disease? Give us a call at (310) 341-4867 to schedule your first appointment today.