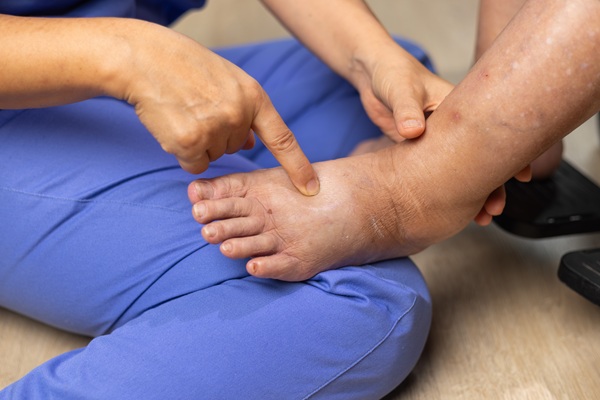
Varicose Vein TreatmentDowney, CA
Varicose vein treatment addresses more than just the appearance of the legs. It is a vital medical intervention for restoring proper circulation and preventing the progression of chronic venous disease. When the veins in the lower extremities become enlarged and twisted, they often signal an underlying problem with the way blood travels back toward the heart.
ProVascularMD provides a comprehensive approach to varicose vein treatment to address these bulging vessels. By utilizing advanced technology and minimally invasive techniques, our team helps patients regain their mobility and comfort. To schedule an appointment, contact our Downey office at (310) 341-4867 today.
What are Varicose Veins?
Varicose veins are vessels that have become permanently dilated and elongated due to a failure in the circulatory system. Inside healthy veins, tiny one-way valves work against gravity to push blood upward. When these valves weaken or suffer damage, blood begins to flow backward and pool in the lower legs, a condition known as venous reflux or chronic venous insufficiency. This pooling creates a high-pressure environment that causes the vein walls to stretch, bulge, and eventually become visible through the skin. While often viewed as a cosmetic nuisance, these veins indicate a significant disruption in the body's ability to move oxygen-depleted blood efficiently.
The symptoms associated with this condition frequently extend beyond the visible blue or purple ridges on the calves and thighs. Many individuals experience a persistent sensation of heaviness, especially after prolonged standing, or a deep ache that worsens as the day progresses. Swelling around the ankles and shins is also a common indicator that the venous system is struggling to balance fluids. In more advanced stages, the constant pressure can cause the skin to become itchy, discolored, or thin. If left unaddressed, this cycle of inflammation can lead to the formation of venous ulcers, difficult-to-heal wounds that require specialized medical attention.
“Varicose veins are vessels that have become permanently dilated and elongated due to a failure in the circulatory system.”
What to Expect During a Varicose Vein Treatment Consultation
A consultation at our office is essential in creating a personalized roadmap for vascular health. The process begins with a detailed discussion regarding daily symptoms, lifestyle factors, and medical history to understand the unique challenges the patient faces. A physical examination allows us to observe the patterns of swelling and any changes in skin texture or color that indicate the severity of the venous insufficiency. This evaluation ensures that the plan addresses the root cause of the discomfort rather than merely treating the visible symptoms on the surface.
Diagnostic ultrasound is the most critical tool we use during this initial meeting to create a real-time map of the leg's internal blood flow and structure. This painless imaging technique allows the specialist to see exactly where the valves are failing and which specific veins are allowing blood to reflux. Identifying the precise source of the pressure allows us to plan a targeted intervention that provides long-term stability.
“Diagnostic ultrasound is the most critical tool we use during this initial meeting to create a real-time map of the leg’s internal blood flow and structure.”
Different Varicose Vein Treatments
Most varicose vein treatments utilize image-guided technology to seal diseased veins through small access points in the skin, avoiding the need for traditional surgery. We will consider the following treatments:
Thermal ablation
Thermal ablation uses either laser or radiofrequency energy to deliver controlled heat to the inside of the damaged vein. This heat causes the vein walls to collapse and seal, allowing the body to reroute blood flow through healthier, deeper vessels. We perform this procedure using local anesthesia, and patients typically experience a significant reduction in pressure almost immediately.
VenaSeal
Medical adhesive, often referred to as VenaSeal, closes the problematic vein. This technique involves the precise placement of a biocompatible glue that instantly seals the vein walls upon contact. Unlike thermal methods, this approach does not require the use of heat or large amounts of numbing fluid, which can be an advantage for some patients. The adhesive remains inside the body and is eventually absorbed as the vein turns into scar tissue.
Foam sclerotherapy
Foam sclerotherapy (Varithena) treats small varicose veins or those remaining after treating a larger source. We inject a specialized foam medication directly into the diseased vessel, guided by ultrasound. The foam displaces blood and irritates the vein lining, causing the vessel to shrink and eventually disappear. This method is especially effective for hard-to-navigate, twisted veins.
Vein stripping
Vein stripping is a traditional surgery and involves creating two incisions on each end of the bulging veins. We then tie off one end, insert a wire into the vein, and pull it out to the other side. This surgery is reserved for severe varicose veins, and due to its nature, we will perform it under general anesthesia.
“Most varicose vein treatments utilize image-guided technology to seal diseased veins through small access points in the skin, avoiding the need for traditional surgery.”
What to Expect During Recovery
Recovery from a minimally invasive vein procedure is typically straightforward, allowing most patients to return to their normal routines the same day. While it is common to experience some mild tenderness or a sensation of tightness along the treated area, these feelings are usually manageable with light activity. Further, we strongly encourage walking immediately after the appointment, as movement promotes healthy circulation in the remaining deep veins. The body begins the process of absorbing the closed vein right away, leading to a gradual improvement in how the leg feels and looks. Most patients find that the chronic heaviness they once felt starts to dissipate within the first few days.
Follow-up care may include the use of compression stockings to support the leg as it adapts to the new patterns of blood flow. These garments provide gentle pressure that helps reduce swelling and keep the treated veins closed during the initial healing phase. We will provide specific instructions on how long to wear these stockings and when it is safe to resume more intense physical exercise. A follow-up ultrasound is often scheduled a week or two later to confirm that the treated veins are fully sealed and that the circulation is moving effectively.
“Recovery from a minimally invasive vein procedure is typically straightforward, allowing most patients to return to their normal routines the same day.”
Benefits of Varicose Vein Treatment
The primary benefit of varicose vein treatment is the dramatic improvement in the quality of daily life through the relief of chronic pain and swelling. When the underlying reflux is corrected, the constant pressure on the leg tissues disappears, allowing the heaviness and fatigue to lift. Many patients will notice that they can stand for longer periods and engage in activities they previously avoided due to discomfort.
Beyond the immediate relief of symptoms, treating venous disease early prevents the progression toward more serious health concerns. By closing the diseased veins, we reduce the inflammatory environment that leads to skin discoloration and permanent thickening of the tissue. This is especially vital for preventing the development of venous ulcers, which can be life-altering and difficult to manage. Addressing these issues early greatly mitigates the risk of complications associated with advanced venous insufficiency.
“Beyond the immediate relief of symptoms, treating venous disease early prevents the progression toward more serious health concerns.”
Questions Answered on This Page
Q. What happens during a consultation?
Q. What are the different varicose vein treatments?
Q. What can I expect during recovery?
Q. What are the benefits of undergoing minimally invasive varicose vein treatment early on?
Frequently Asked Questions
Q. How does varicose vein treatment differ from treating spider veins?
A. Varicose veins are large, bulging vessels that often indicate a significant problem with the internal valves and the overall pressure in the leg. Spider veins are much smaller, thin lines that appear close to the surface and are usually considered a cosmetic concern rather than a major circulatory issue. While the treatments for both involve closing the diseased vessel, varicose vein treatment typically requires addressing a deeper source of reflux to be successful.
Q. Is an ultrasound necessary before deciding on a treatment plan?
A. Diagnostic ultrasound is the most important part of the evaluation because it allows us to visualize the direction of blood flow in the leg. Without this mapping, it is impossible to know which veins are failing and where the pressure is coming from. The ultrasound ensures that the treatment targets the actual cause of the problem rather than just the visible symptoms.
Q. Will the blood have trouble flowing if a vein is closed?
A. When a diseased vein is closed during a procedure, the body naturally and immediately shifts the blood flow to healthier, deeper veins in the leg. Most people have an abundance of veins, and the ones being treated are already failing to efficiently move blood toward the heart. Closing these problem vessels improves overall circulation by eliminating the pooling and pressure that previously hindered the system.
Q. Can these treatments be performed without general anesthesia?
A. Only the vein stripping procedure uses general anesthesia. However, considering all other procedures are minimally invasive, we typically perform them using local anesthesia and topical numbing. Sometimes we may use a light sedative to ensure the patient remains completely comfortable during the procedure. This approach avoids the risks and long recovery times associated with general anesthesia or traditional hospital stays.
Q. Does the treatment help with the itching and skin changes?
A. Treating the underlying venous reflux is highly effective at reducing the inflammation that causes the skin to become itchy and discolored. When the high pressure inside the veins is eliminated, the skin and soft tissues are no longer subjected to constant irritation. While some long-term skin changes may take time to fade, the reduction in pressure prevents further damage and creates a much better environment for healing.
Call Us Today
A successful approach to vascular health management depends on taking a proactive stance on circulatory problems before they become a medical emergency. Fortunately, ProVascularMD offers a varicose vein treatment at our Downey office. To schedule an appointment, contact us at (310) 341-4867 today.